One of the most important administrative tasks that healthcare professionals and organizations must stay on top of is ensuring that their physician credentialing and healthcare certifications are always accurate and up to date.
However, with increasing amounts of administrative time and paperwork involved in the medical credentialing process, it can become a significant burden on healthcare facilities.
Any small mistake or oversight can lead to a lapse in certification of a healthcare professional, resulting in issues with insurance payments for services already provided. Let me explain how this process works and why it’s critical for all medical services.
What is Physician Credentialing?
Physician credentialing is a certification process that verifies all professional records relating to a healthcare professional’s training, education, licensing, and experience. It’s a vital requirement for doctors, surgeons, nurse practitioners, and many other professionals who directly and indirectly deal with medical patients.
While the medical provider credentialing process varies between different medical professions, the concept is the same. The goal is to obtain a professional certificate that confirms the individual has received all the necessary education and training to practice medicine.
It’s also a way for healthcare organizations to validate the skills and experience of new and existing employees.
We will outline the multiple benefits of healthcare credentialing shortly. But the most important reason for staying up-to-date with medical credentialing is that insurance companies can withhold payments if any certificates are not current.
It’s also important to understand that medical credentialing is not a one-time process. Most medical professionals will have to go through a credentialing process every three years.
Benefits For A Healthcare Provider
There are several key benefits for healthcare professionals when they are able to stay on top of their credentialing. And it’s not all just about having a certificate for the office wall.
Patient Confidence and Trust
Trust plays a crucial role in every doctor-patient relationship, and unfortunately, it is often taken for granted. Even more important, it can be very difficult to build up that trust with people who might be going through a very traumatic time in their life,
For all healthcare providers, it’s critical to do everything possible to demonstrate that all employees providing medical services are fully credentialed.
It immediately shows new and existing patients that staff have the education, training, skills, and experience necessary to help them get better. And the more trust you can build up right from the start, the more confidence they will have to go ahead with recommended treatments.
Higher Professionalism
While there is a lot of paperwork involved in medical credentialing, this is a time and effort investment that can instantly pay off by providing healthcare facilities with a professional appearance.
It also shows patients and vendors that you care enough about the education and experience of medical staff to make the effort needed to achieve and show off all the credentials.
Seeing a certified document as proof that all credentials have been professionally verified is simply something you can’t do without. And you don’t want to end up in a situation where patients or an insurance company ask for credentials and you are unable to provide them.
Reduced Medical Errors
According to research statistics, medical errors are involved in almost 100,000 deaths in America each year. That’s a staggering number that is down to many different reasons.
However, healthcare providers can protect themselves from becoming a significant part of such statistics by ensuring that all staff are always fully up-to-date with their credentialing. Only with the proper supporting documents that confirm a provider has the necessary training and education will such credentials be issued. And because all documents must be up-to-date to renew credentials, it can help healthcare providers avoid hiring medical staff who may not meet all the requirements. More on these shortly.
Ensure Timely Payment
One of the most immediate impacts of medical credentialing is the direct effect on revenue and cash flow for a medical services provider. And it all comes down to the contracts between medical providers and insurance companies.
These contracts include clauses to specify that reimbursements are dependent on all medical practitioners involved in a treatment having fully up-to-date credentials. This means that if there is an issue with renewing credentials on time or if a filing mistake leads to delays in receiving credentials, then insurance companies will withhold payments until the matter is resolved.
From the perspective of the healthcare practice, keeping provider credentials current isn’t just a regulatory checkbox. It’s critical for operations, reimbursement, liability management, and maintaining a good reputation.
Why Credentialing Matters to Healthcare Practices
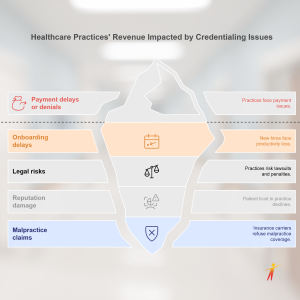
- Direct Impact on Revenue
Most insurance companies, including Medicare and Medicaid, require current and verified credentials for providers to be reimbursed. If a provider’s credentialing lapses, the practice may be unable to bill for that provider’s services. The Centers for Medicare and Medicaid Services (CMS) can deny payments retroactively if they discover expired credentials.
A 2021 MGMA poll found that 63% of practices reported payment delays or denials due to credentialing issues, most commonly because of incomplete or outdated information.
- Delays in Onboarding and Lost Productivity
Credentialing can take 90 to 150 days, depending on the payer’s specific requirements. If a new hire’s credentials aren’t submitted on time or incorrectly, they can’t see patients, resulting in weeks or months of lost productivity. This is especially painful for smaller practices or busy specialties, such as orthopedics or dermatology, where provider schedules are often booked weeks in advance. - Legal and Compliance Risks
Allowing an uncredentialed provider to deliver care can expose a practice to lawsuits and regulatory penalties. In some states, this is considered practicing without a license—an offense with serious legal consequences. - Damage to Reputation and Patient Trust
Patients must trust that their provider is licensed and qualified. If word gets out that a provider’s certification lapsed—or worse, they were disciplined and it went unnoticed due to lax credentialing—confidence in the entire practice can plummet. - Increased Risk of Malpractice Claims
Insurance carriers may refuse to cover a malpractice claim if a provider’s credentials are not current at the time of the incident. This not only jeopardizes the provider but also leaves the practice financially exposed.
Credentialing isn’t just the provider’s responsibility; it’s a business-critical function that should be tracked and managed with the same diligence as patient billing or compliance. Many practices now outsource credentialing to specialized partners to avoid the administrative headache and costly consequences of falling behind.
Keeping credentials up to date means:
✅ Getting paid on time
✅ Minimizing legal exposure
✅ Ensuring uninterrupted patient care
✅ Preserving your reputation
When it comes to credentialing, an ounce of prevention is worth thousands in revenue, hours, and peace of mind.
How Does The Medical Credentialing Process Work?
The physician credentialing process is a time-consuming administrative task that requires training and experience to ensure all requirements are in proper order and available for review. For many organizations in the medical industry, this means allocating administrative staff to stay on top of this vital business practice.
Credentialing Prerequisites
While there are differences in the medical credentialing process from state to state, as well as for different professions, there are some typical items that you have to check off before you make an application.
Here are the most important ones:
• Certificates of education and training
• Medical board certifications
• Work history and experience
• Full history of clinical privileges
• Contact information for employment references
• Clinical performance reviews
• Medical malpractice insurance claims history
• Professional licensing certificates
Some of this information, like education certificates, won’t change much over the years. But, keeping track of clinical privileges and your work history is more difficult to manage.
That’s why it’s important to keep notes about any changes in these areas so that you have all the necessary details when it comes to renewing credentials.
Application And Processing
Once you have collected all the necessary details, it’s time for a healthcare provider to validate. This may involve verifying primary sources for new employees to ensure that their previous experience and training records can be substantiated.
An application, along with all the supporting documentation, is then submitted for the appropriate verification, where it’s reviewed and verified. Depending on the work history and amount of training throughout a career, this process can be quite time-consuming.
This application process also involves reviewing any registered complaints against medical practitioners that may have previously been registered.
Recredentialing
Medical provider credentialing is not a once-off process. In most cases, medical staff have to go through a re-enrollment process every three years in order to keep their credentials up-to-date. All existing holders of credentials will receive notification when they are due for renewal. But as with many such notifications, people often leave it too late, or they miss them altogether.
That can lead to lapsed credentials and a stressful time to rush through the process. That’s why it’s important to either have dedicated admin staff to stay on top of such tasks or to outsource credentialing to DataMatrix.
Outsource The Credentialing Process With DataMatrix Medical
Credentialing is a vital administrative business process but one that involves a lot of time and paperwork. And because small mistakes in the handling can lead to long delays, it’s important to have someone experienced in the process available.
Most healthcare providers attempt to handle this in-house, but it can result in significant administrative overhead.
That’s where outsourcing physician credentialing to DataMatrix becomes a huge time and cost-saving. Not only will this ensure that you always stay on top of your credentialing requirements, but it will also free up your administrative staff to focus on other important tasks that support patient care.
Call us today to find out how we can streamline your entire credentialing process. Learn about how you can pair our services. From medical transcription to prior authorizations, we offer services to keep your practice running efficiently!

Nathaniel Smathers is the VP of Client Education and Marketing. He is also a long time contributor of the DataMatrix Medical blog and has a background in healthcare content creation for over a decade. Nathaniel is passionate about exploring the intersections of healthcare, data analysis, and digital innovation.